
by Abu Bakar Bin Alam,
23 April, 2026
In the vast, braided reaches of the Brahmaputra River, the landscape is defined by its refusal to stay still. For the millions of people living on “chars”—shifting silt islands created and consumed by the river’s current—permanence is a luxury. In these remote areas, where the nearest medical facility may be a day’s journey across water, healthcare is often a matter of access rather than availability. It is within this context of environmental and social isolation that the EFH Friendship Hospital (EFH) operates as a vital lifeline.
The story of EFH is one of evolution and steady expansion. While Friendship’s journey began in 2002 with the Lifebuoy Floating Hospital (LFH), the launch of EFH in 2008 marked a critical turning point. It was the first scale-up of the model, proving that mobile, river-based healthcare could be replicated and sustained. Since then, the EFH has served more than 750,000 patients through over one million health service interactions. Today, the EFH is a cornerstone of a fleet that has grown to seven operational floating hospitals, each a testament to a commitment to reach the unreachable.
A model solution
The impact of EFH lies in its integration within Friendship’s 3-tier healthcare system. The hospital does not simply wait for patients to arrive; it is the surgical heart of a grassroots network:
Tier 1: Friendship Community Medics (FCMs): Local women trained to provide primary care and health education within their own communities.
Tier 2: Satellite Clinics and Health Camps: Mobile teams that rotate through the chars to provide specialised screenings and basic diagnostics.
Tier 3: Floating Hospitals: The specialised hub where secondary care, including complex surgeries and long-term treatment, takes place.
This system ensures that the most marginalised individuals are identified at the doorstep and guided through a continuum of care that culminates in the advanced facilities of the EFH.
| Patients Served | Health Services | Surgeries | Consultations | VIA Screenings | Sensitised | Medical Camps |
| 750,000+ | 1,100,000+ | 20,000+ | 11,000+ | 66,000+ | 112,500+ | 450+ |
In a normal operational year, EFH aims to serve over 54,000 patients and deliver more than 85,000 health services. The hospital plans to conduct 30 specialised surgical camps annually, covering eye, orthopaedic, reconstructive, visceral, and gynaecological procedures, delivering over 1,300 surgeries.

Restoring Dignity and Vision
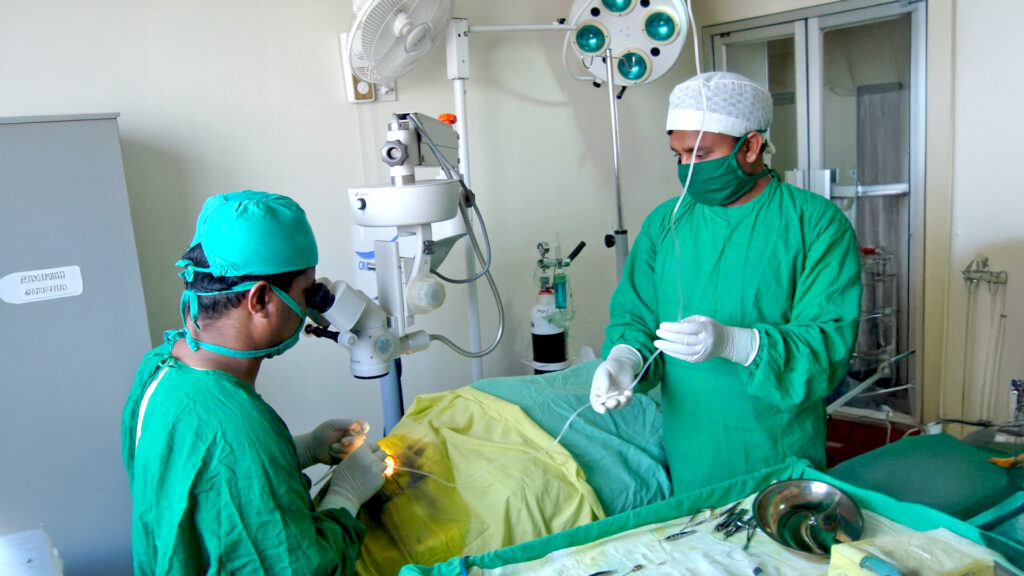
The clinical work aboard EFH is focused on life-changing interventions that address both immediate suffering and long-term economic exclusion. Ophthalmic care remains a primary focus; in these riverine regions, a simple cataract can lead to total blindness, rendering an individual a burden to their family. On EFH, specialised surgical teams perform suture-less cataract procedures that take less than twenty minutes but restore decades of independence.
The hospital also serves as a sanctuary for those with physical disabilities. Through specialised orthopaedic camps, children with congenital conditions like clubfoot or those suffering from the long-term effects of polio receive corrective surgeries. These are often children who have never walked or attended school. By bringing paediatric surgeons and post-operative care directly to the char communities, EFH bridges the gap between a life of isolation and a future of opportunity.

Resilience in the face of climate change
The climate crisis compounds the necessity of EFH. As rising sea levels and intensified monsoons increase the frequency of flooding and erosion, land-based infrastructure is often washed away. A floating hospital, however, is inherently resilient. It moves with the water, following the communities it serves.
Data from peer-reviewed studies and reports from the Pulitzer Centre highlight that as environmental shifts displace populations, mobile infrastructure becomes the only viable method of delivering consistent service. EFH is equipped with two operating theatres, an eight-bed ward, a dental unit, and a full laboratory, ensuring that the quality of care in a remote char is comparable to a regional urban centre.
According to Friendship’s 2024 household survey in its operating areas, 30% of residents live below the extreme poverty line of USD 2.15 per person per day, while the remainder are classified as the general poor.
While the challenge of riverine healthcare is immense, the EFH remains a steady presence. It is a model built on the belief that neither geography nor cost should be a barrier to dignity. Through quiet determination and a proven system of tiered care, EFH continues to navigate the shifting waters of the Brahmaputra, ensuring that hope remains afloat for those whom the rest of the world has often forgotten.



